Canadian health-care workers tapped into millions of OT hours during COVID-19 pandemic

Posted October 20, 2023 7:37 am.
Last Updated October 20, 2023 7:41 am.
As health-care workers continue to leave the profession due to burnout and being overworked, we’re receiving a better understanding of how it’s impacting their well-being and that of their patients.
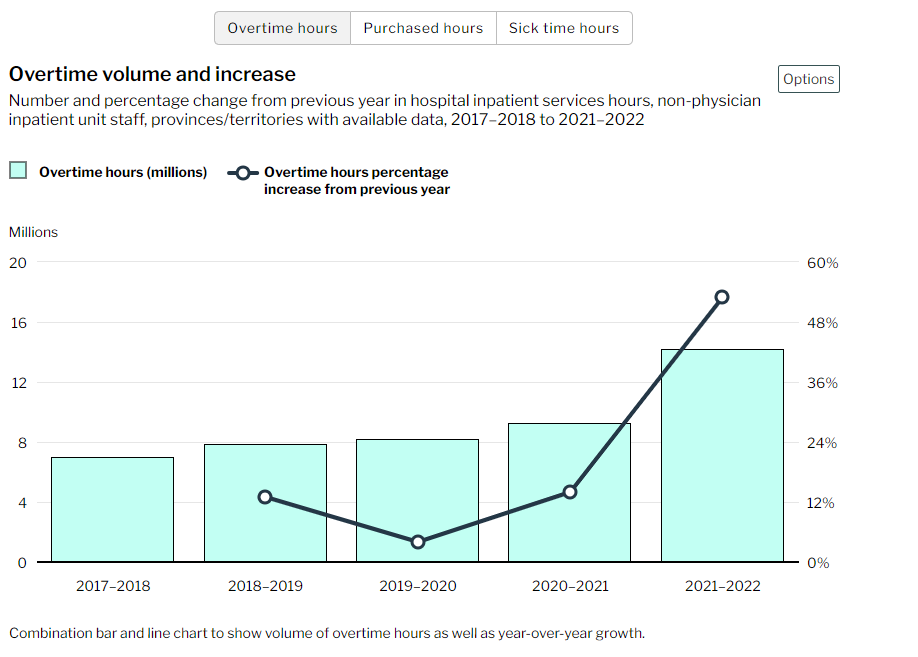
A new report from the Canadian Institute for Health Information (CIHI) shows that during the height of the COVID-19 pandemic, which was 2021-2022, staff in inpatient units at hospitals all across the country logged 14 million overtime hours.
“If you were to equate that to people working, say, the equivalent of a full-time job, people who are already employed were working the equivalent of over 7,000 extra full-time jobs,” explained Kate Parson, program lead for Health Human Resources at CIHI.
She says one concern highlighted by this report is the detrimental impact on the most vulnerable people. “… [it] could disrupt patient care or sometimes decrease the quality of care, just because of system-level issues,” she explained.
Parson adds it’s not just the burnout factor for healthcare workers, adding they’ve seen an increase in physical ailments among them as well, including ulcers, pneumonia, and UTIs.
“Throughout the COVID-19 pandemic, nurses working in the hospital sector increasingly reported experiences of burnout, moral distress, and a desire to leave the profession. In 2022, the number of registered nurses working in hospitals and providing direct care to patients declined slightly, by 1 per cent (828 fewer RNs),” the report noted.
“In the same year, Statistics Canada reported 95,800 vacant nursing, personal support worker and health care worker jobs, a record high for the industry.”
The CIHI says there was also an 80 per cent increase in the number of purchased hours, from 850,000 in 2020-2021 to more than 1.5 million the following year.
Another issue raised by the industry is staff willing to leave their current role for less stress and better pay.
“In 2022, the number of RNs that were self-employed or working for private nursing agencies increased by 6 per cent (867 more RNs). Contracts with private agencies offer higher rates of pay and more flexibility in scheduling, which was commonly noted as desirable among nurses during the pandemic.”
Parson hopes that given all the compiled information, changes come to the health-care system.
“Supporting the retention of staff employed by publically funded hospitals is key and we know that there are some strategies already in place to improve things like flexibility for staff, ongoing mental health supports, opportunities to advance, to ensure those experienced staff stay in place.”
Last year, the B.C. government said it was tackling the global health-care worker shortage through a new provincial strategy that included major investments in recruitment and retention. The changes were launched following an independent review of the province’s health-care system.